Sleep Behaviors and the Shape of Subcortical Brain Structures in Children with Overweight/Obesity: A Cross-Sectional Study
Are Subtle Brain Changes the Hidden Cost of Poor Sleep in Kids with Obesity?
In the past decade, studies have shown that nearly one-third of the pediatric population experiences inadequate sleep. This randomized controlled trial unveils how sleep behaviors shape the developing brains of children struggling with overweight or obesity. Using advanced 3T MRI and shape analysis of subcortical brain structures, researchers examined 93 right-handed children (mean age 10 ± 1.1 years), all presenting with overweight or obesity and no diagnosed psychological or physical conditions, to assess whether variations in sleep patterns influence the brain beyond just rest and recovery.
The key findings pointed to the bilateral pallidum and the right putamen—critical components of the basal ganglia, which are involved in motor control, habit formation, and executive functions. According to this research, longer time spent in bed in developing children is associated with shape expansions in these regions. Notably, no significant shape differences were found in the hippocampus, amygdala, caudate, or thalamus. This underscores the specificity of the putamen and pallidum findings and highlights the potential vulnerability of the basal ganglia in overweight children with disrupted or extended sleep cycles. These alterations may reflect early stress responses, behavioral regulation shifts, and adaptive brain development.
Overall, the study offers compelling evidence that sleep behaviors are not only crucial for rest but also for supporting optimal brain development in children vulnerable to obesity-related risks.
Remodeling and Repair of the Damaged Brain: The Potential and Challenges of Organoids for Ischaemic Stroke
Organoid Transplantation – Just Another Stem Cell Innovation or Revolution in Neural Regeneration?
Ischemic stroke is the leading cause of neurological dysfunction in clinical practice. However, due to multiple factors such as limited treatment options that are hindered by pathological barriers and inability to seek timely treatment, extensive necrosis in the infarcted area can occur – leading to irreversible neuron damage in the brain.
This study explores neuroplasticity and its mechanisms during the post-stroke recovery period, including cellular responses and potential new treatment strategies that utilize regenerative medicine and cell remodeling.
Emerging neural regeneration paradigms offer trailblazing answers – especially stem-cell based methods: stem cell therapy that utilizes stem cells in differentiating into neural cells via multiple pathways – that also increase the functional outcome, yet it comes with its challenges, e.g., limited survival of transplanted cells and poor integration. A revolutionary alternative has entered the scene – cerebral organoids. Stem cells are also used in this method to create these 3D organoids that mimic the workings of the brain and its development. They have the ability to restore function by integrating with host neural circuits, forming synapses, and stimulating neurogenesis and angiogenesis. Compared to traditional stem cells, organoids possess complex cellular environments and have better sustainability post-transplantation.
However, all of this comes with a moral conflict and an ethical discussion to build on regarding many aspects, such as the origin of stem cells and public reaction, and acceptance of the method and its workings. Organoid transplantation is a field to be explored, but the need for further research to improve the method, its timing, and its safety remains.
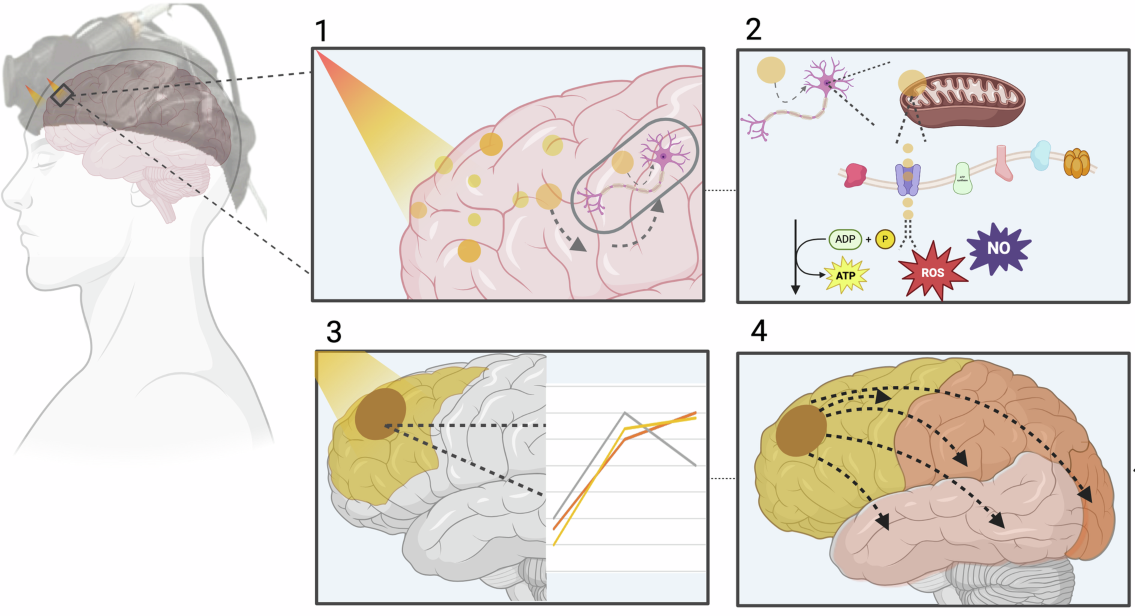
Transcranial Photobiomodulation Improves Functional Brain Networks and Working Memory in Healthy Older Adults: An fNIRS Study
As our brain networks weaken with age, what if it were possible to rebuild them using light?
In their 2025 study, Yang and colleagues addressed this question by investigating the cognitive effects of transcranial photobiomodulation (tPBM) in healthy older adults. They employed functional near-infrared spectroscopy (fNIRS), a non-invasive method that measures cortical blood oxygenation changes reflecting brain activity during cognitive tasks. Following the tPBM application, significant enhancements in functional connectivity—particularly in the prefrontal cortex—were observed. These neural changes were accompanied by marked improvements in working memory performance, as measured by the n-back task. The findings suggest that this non-invasive, light-based intervention may positively influence cognitive aging processes. This study demonstrates that light-based interventions to support cognitive function could potentially pioneer new frontiers in the neuroscience of the future.
Novel Blood-Based Proteomic Signatures Across Multiple Neurodegenerative Diseases
Does Blood Hold the Clues to Brain Degeneration in Dementia?
This study introduces a highly sensitive blood-based proteomic approach—NULISA (Nucleic Acid Linked Immuno-Sandwich Assay)—that can detect disease-specific biomarker signatures for neurodegenerative diseases such as Alzheimer’s disease (AD), frontotemporal dementia (FTD), Lewy body dementia (LBD), and progressive supranuclear palsy (PSP).
Proteomic analysis was performed on blood samples from 172 individuals. The results were remarkable: serum neurofilament light chain (NfL) was elevated across all disease groups and predicted faster decline and shorter survival. Corticotropin-releasing hormone (CRH), unexpectedly decreased in patients, was also correlated with poorer prognosis. From diagnostics to survival prediction, this multiplex platform may soon rearrange how clinicians detect, monitor, and treat different forms of dementia.
What sets this study apart is that, normally, in neurodegenerative diseases and their disease-specific fingerprints cannot be used for detecting the heterogeneity of the disease. But now clinicians can detect the biological heterogeneity of the disease with NULISA easily. Unlike the regular diagnostic methods like CSF and PET imaging, this method offers easy use and is cost-effective for routine clinics.
Learning to Read During Adulthood Improves Memory, Executive Functioning and Brain Connectivity: Results from the PROAME Study
Back to School: Does Learning to Read As an Adult Show a Positive Effect on Neurodegenerative Diseases?
Whichever organ you use less, its abilities will regress. That of course includes the human brain and memory. Illiteracy is a known risk factor for dementia. This PROAME study (Promotion of Adult Memory and Education) covers the correlation between acquiring the ability to read and the brain’s cognitive functions and connectivity.
108 illiterate adults over the age of 40 from Brazilian public adult schools were put through longitudinal controlled trials. The intervention group received targeted literary training in addition to the regular “adult education” that all participants received.
In result of cognitive assessments, plasma neurofilament light chain (NfL) levels, and brain MRI being conducted at baseline and at six months, some changes were observed in the participants: In the 77 participants that completed the follow-up assessment, mainly change in episodic memory, accompanied by changes in executive functions and minor differences in other factors that were being assessed. Although episodic memory improved in both groups, executive function in the intervention group was shown to improve more drastically following some adjustments in the covariates.
Overall, the study touches on how adult literacy training can be utilized in enhancing cognitive resilience and dementia prevention.
Antidepressant and Antiobesity Drug-Induced Serotonin Syndrome Complicated by Multiple Organ Injury: A Case Report

Can the combination of different drugs cause multiple organ injury?
Depression and obesity are among the most common health issues today, and the use of antidepressants and anti-obesity medications in their treatment is increasing. This case report thoroughly examines serotonin syndrome induced by the concurrent use of antidepressant and anti-obesity drugs, along with the resulting complication of multiple organ injury.
In this rare but potentially life-threatening case involving a 45-year-old female patient, neurological symptoms associated with serotonin syndrome were accompanied by multiple organ damage. Based on clinical evaluation and laboratory findings, a prompt diagnosis was made, and the treatment process was managed with a multidisciplinary approach. This case report highlights the importance of careful monitoring by healthcare providers regarding serious pharmacological interactions that may arise from the combined use of different medications.